Throughout the pandemic, there’s been an understanding that COVID-19 testing could be key to getting back to normal. It’s quick and easy, it eliminates worry and ultimately, it saves lives. As an events industry, investing in testing can demonstrate that our events (once they’re allowed to resume) are really and truly safe.
But what kind of tests should you invest in? Is there anything you should watch out for? We’ve laid it all out here.
Testing checklist
- Use testing methods that are seen as ‘Gold Standard’ by the WHO.
- Steer clear of tests that are using new and unproven technology.
- Make sure any tests you buy have the right certification.
- Check that the tests you’re interested in are actually in production and available.
- Check the ‘Limit of Detection’ to make sure a test can identify asymptomatic carriers.
- Be aware of a test’s specificity and sensitivity, rather than just going by accuracy claims.
- Beware of tests that contain proprietary hardware, as this means there’s only one source of supply (plus, they can be expensive).
- Check whether the test needs special handling and whether that’s achievable (eg. it might need cold storage).
- Don’t be influenced by press announcements about procurement contracts. Often, these contracts are subject to certification and proof of performance, which may never arrive.
What is WHO’s ‘Gold Standard’?
WHO Gold Standard tests are those that have been recognised by the World Health Organisation as the best available. In other words, they’re established testing methods that are based on proven techniques.
As there’s agreement in the scientific community that these methods are likely to be the most reliable, we’d recommend using testing methods that have been recognised in this way, rather than unproven methods. After all, these people know what they’re talking about. That said, we’re not scientists so please don’t take our advice as golden!
Types of test
There are two main groups of tests – tests that can identify whether someone currently has the virus; and tests that can identify whether someone has had the virus in the past (like Antibody tests and Antigen tests).
We’ll focus on the first kind here, as finding out whether someone is currently infected will allow you to screen people for entry to your event. There are two main types available:
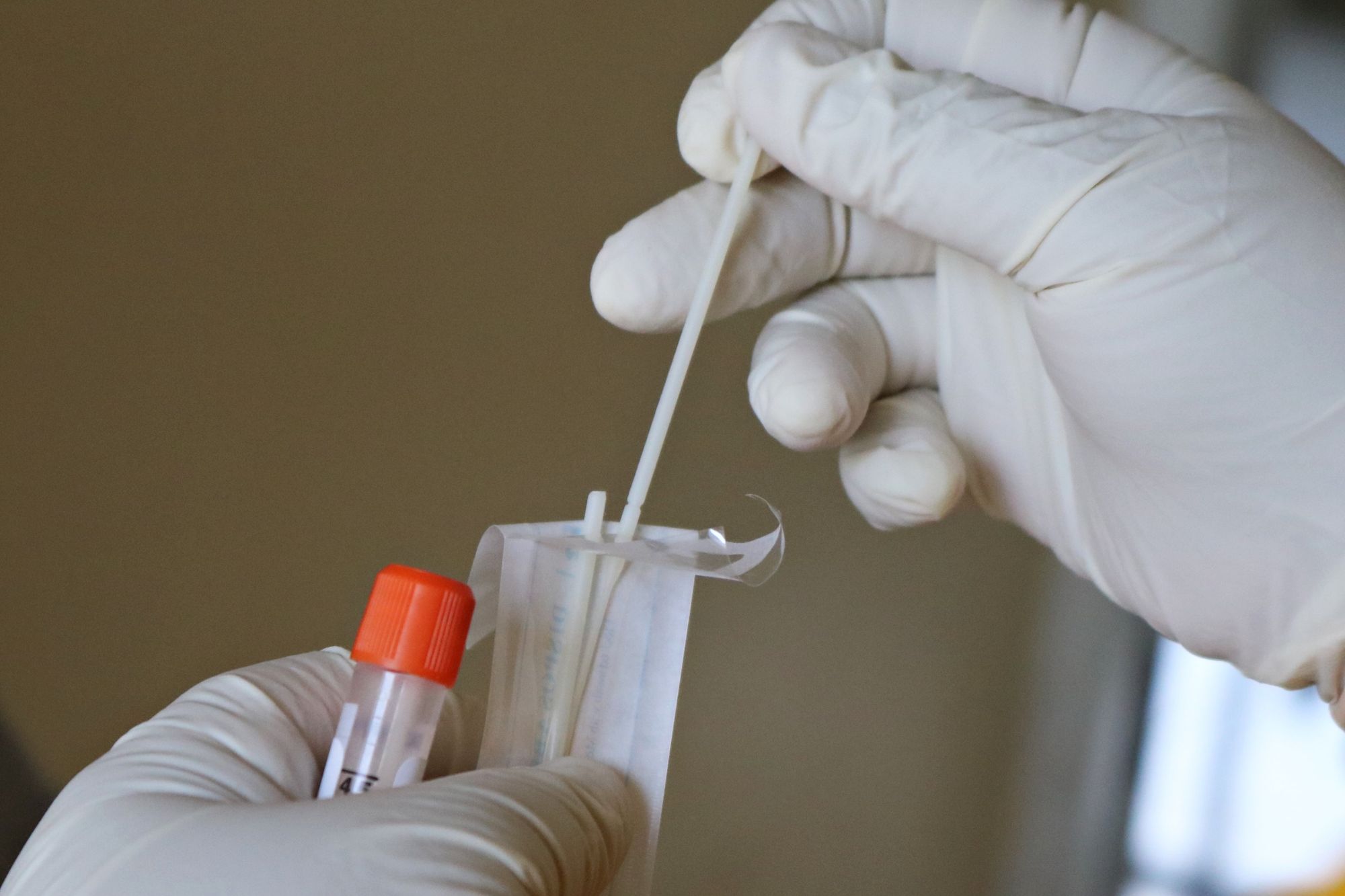
RT-PCR
This test involves a swab to the nose and throat, which is then analysed in a lab. The test looks for viral genetic material to find out whether someone is infected. PCR is a common scientific method that’s been used to detect genetic information for around 20-30 years.
Pros:
- WHO Gold Standard method.
- Generally reliable and accurate.
- Tried and tested method.
- Suitable for screening.
Cons:
- Can only be processed in a lab (so can’t be completed on-site).
- Turnaround is between 24 and 72 hours.
- Can create a biohazard, for instance in transport
RT-LAMP
This test also needs a nose and throat swab, but this time it’s mixed with a buffer and placed into a machine for isothermal amplification. This means that the viral genetic material can be analysed more quickly.
Pros:
- WHO Gold Standard method if it incorporates a Nucleic Acid Amplification Test (NAAT).
- Turnaround is usually between 30 and 90 minutes, depending on the test.
- Can be carried out on-site.
- Doesn’t create a biohazard.
- Generally reliable and accurate.
- Suitable for screening.
Cons:
- Doesn’t indicate if you have any immunity.
- Tests that don’t incorporate a NAAT are not WHO Gold Standard.
Certification
Although the information we’ve outlined above should give you a broad idea of what kind of test you’re looking for, there are lots of different tests that fall under these categories. You’ll need to make sure that any tests you’re considering have the right certifications. Here’s what you’ll want to look for.
- CE: This shows that tests conform with health, safety and environmental protection standards for products sold in the EEA, and that they have been reviewed by three regulated labs. Tests marked as CE get a ‘Free Sales Certificate’ that allows them to be sold in the EEA.
- IDVR: Coronavirus tests are subject to In-Vitro Diagnostic Regulations. In the EU, you can tell that these regulations have been met because the tests should have a CE-IVD certificate. Without this, they can’t be legally sold.
- ISO: The International Organisation for Standardisation (ISO) is an organisation that develops standards for quality, safety and efficiency. The ISO certification confirms that tests meet their standards for quality assurance.
- MHRA: The Medicines and Healthcare products Regulatory Agency (MHRA) is responsible for making sure that medicines and medical devices are safe and effective in the UK. Other countries will have their own regulatory bodies, such as the FDA in the US or the AEMPS in Spain.
Limit of Detection
The Limit of Detection (LOD) refers to how much of the virus is required to trigger a positive test result. The higher the LOD, the more positive cases the test is likely to miss, as it won’t be able to pick up lower levels of the virus.
People who are asymptomatic, or who are in the pre-symptomatic phase of infection, may have a lower viral load than others. Being able to detect infection in these people as early as possible is important to establish a COVID-free zone at events.
Isothermal amplification tests (the RT-LAMP type tests we mentioned earlier) are particularly good at picking up low viral loads, so they could be a good shout when you’re looking to screen people for entry into your event.

Accuracy
When you’re considering how accurate a test might be, there are two main things to look at: specificity and sensitivity.
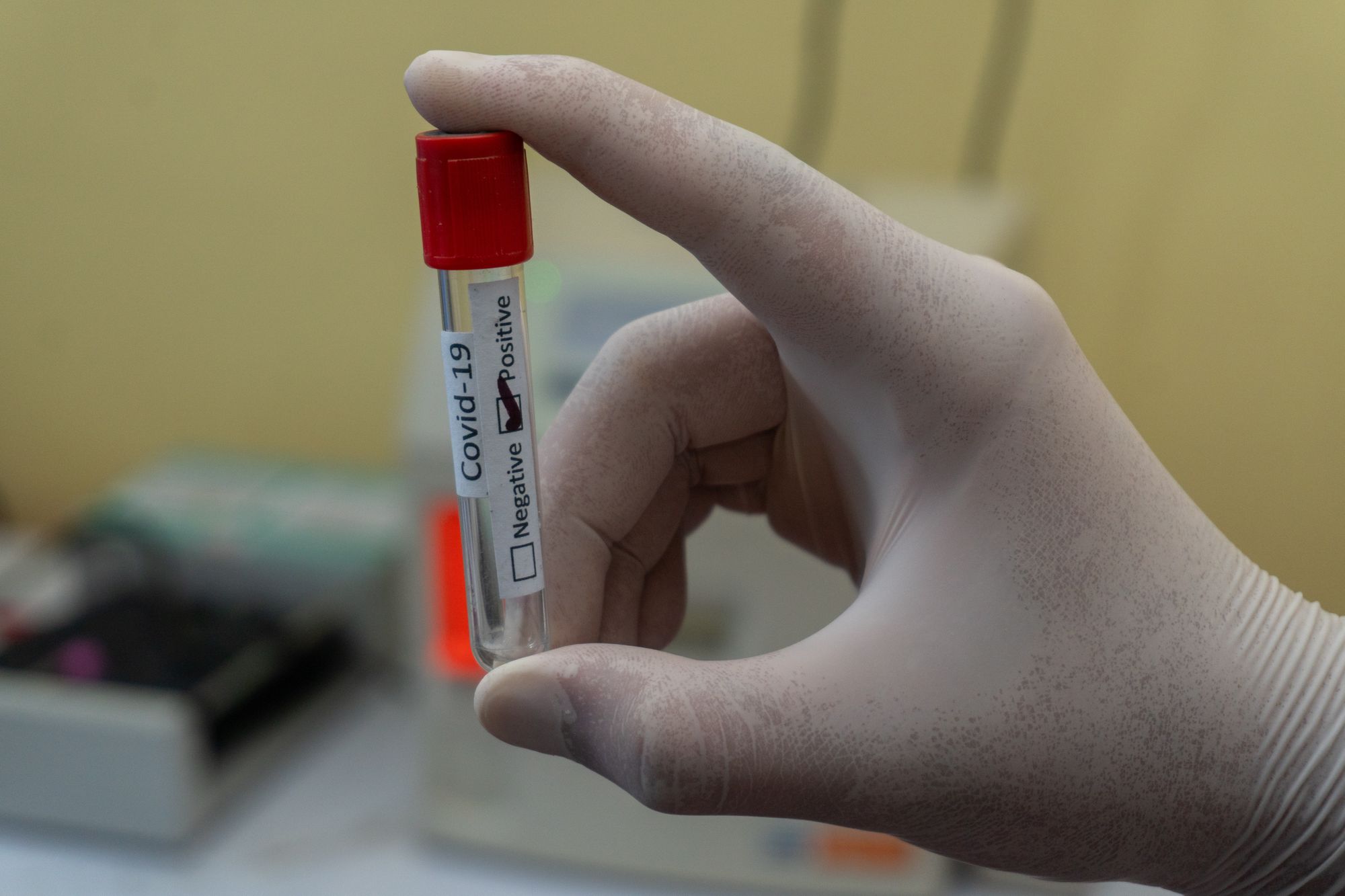
- Specificity: This is the percentage of people who don’t have COVID-19 who accurately receive a negative test. A test that has a specificity of 100% has no false positives.
- Sensitivity: This is the percentage of people who are infected with COVID-19 who accurately receive a positive test. A test that has a specificity of 100% has no false negatives.
Generally, you want to pick a test that has high levels of sensitivity, although specificity is also important.
That said, often tests will state their accuracy based on the window in which they perform best. For example, a test might say it has 98% specificity, but if someone took the test outside of the 7 days after receiving symptoms, that figure could fall to 70%.
This is a little worrying given the fact that people could be most contagious during the 15 days before they display symptoms. So, make sure you interrogate any claims of accuracy and measure it up against the LOD.
Speed
When it comes to screening, it makes sense that tests that produce results quickly will be the most effective. After all, if there’s a gap of a few days between taking the test and getting the results, it’s possible that people could get infected during that window.
However, don’t become sold just because a test claims to have a really quick turnaround. These claims can be misleading.
For example, there was recently a test that got a lot of coverage in the press because it claims to take just 20 seconds. While that does sound very fast, this test uses its own machine to generate results, and this machine can only take one test at a time. A standard 96-well PCR machine takes closer to 30 minutes to generate a result, but it can handle 72 tests at a time.
Given the extra preparation time it takes to handle one test at a time, you could actually handle more tests in a 24-hour period using the PCR machine. On top of this, many tests that claim to be ‘super-fast’ use experimental technology that may sacrifice accuracy in favour of speed.
All this goes to show that you need to look carefully at claims of speed and apply the information to your own needs and circumstances.
When it comes to screening, there are so many tests out there that it can be difficult to know where to start. But once you’ve thought carefully about your priorities and narrowed down the options to those that are tried, tested and proven to work, things get a lot easier.
That said, in the interests of transparency, a little disclaimer: we’re not scientists or medical professionals. For more detailed information about Coronavirus testing methods and devices, head over to the EU Science Hub or The Centre for Evidence-Based Medicine.
If, on the other hand, you’re ready to learn more about planning a Safer Event, we can help. Download our Safer Events white paper or find out how to become accredited as a Safer Events organiser. We will meet again!




